Although the Ministry of Health of Saudi Arabia has been successful in managing and containing Covid-19 to date, existing plans and strategies that were developed during previous disease outbreaks, may not fully meet the needs of the Kingdom, especially for non-Covid-19 patients requiring treatment. There is, however, a great opportunity to use the Kingdoms emerging cluster model to dynamically balance the needs of Covid-19 patients with wider population healthcare needs particularly for patients with urgent conditions (e.g. abdominal aortic aneurysms) and those showing early symptoms (e.g. suspected sarcomas), where delays in treatment and diagnosis could lead to poorer outcomes.
As the country starts relaxing restrictions, each change in these social interventions brings with it the risk of new outbreaks or spikes in transmission, leading to targeted re-establishment of restrictions. For the health sector, this presents challenges as providers reestablish normal service provision and subsequently revert back to emergency measures to focus on the next wave of Covid-19 patients. Over the coming weeks or months, the health sector could find itself managing an unusual infection curve
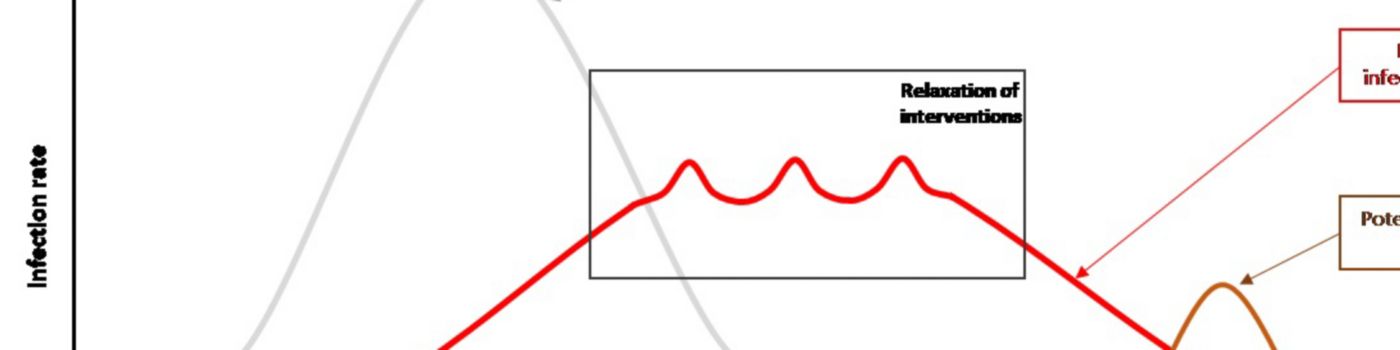
The Vision 2030 transformation program of the Ministry of Health provides the Kingdom with a new approach to the management of health systems, decentralizing decision-making and allowing local health systems to shape care provision to meet the needs of their population. This agility will be crucial during an extended period of response where infection rates could fluctuate significantly as local outbreaks occur.
Existing clusters should be reviewing the demand for Covid-19 related care for their population and strategically stepping up, and down, capacity as required. This tactical planning and operational management should categorize facilities into three categories:
- Covid-19 response centers (hot sites) dealing with the majority of the demand
- Emergency centers, hospitals providing step down care and possibly non-covid-19 trauma care, but able to quickly switch to become response centers when infection rate thresholds increase above agreed thresholds
- Elective centers, focused on maintaining a level of elective care for urgent patients, these will be the last facilities to be used for Covid-19 response
The benefits of segmenting facilities and phasing the response include the creation of a center of excellence for the management of Covid-19, the ability to rotate staff between facilities to reduce stress and exhaustion of staff, and the reduction in unnecessary mortality due to limited access to urgent elective treatment. This planning and operational approach is more suited to the extended duration expected with Covid-19 and is fully aligned to the transformation program, potentially supporting the acceleration of implementation by initiating new ways of working (e.g. pooled waiting lists, managed clinical networks).
For those health systems not yet operating in the cluster model there is a clear opportunity to take greater ownership of the management of Covid-19 to shape the response to meet their population’s needs whilst maintaining some core service provision.
Even if all facilities are currently fully utilized to manage the immediate Covid-19 response, developing a clear plan with designations and thresholds for hospital facilities will provide a tactical framework for the clusters during the extended response period. This planning will also form the basis of the return to normal for the health system, providing a structured approach to the management of the recovery phase.
Post-Covid-19, the planning and the developed operational models, could also form the basis of a suite of initiatives that integrate care provision across clusters and reshape the provision of care to create planned surgery centers and trauma centers that drive improvements in quality and outcomes.
These plans could be quickly developed through a rapid assessment of health economies, with learning taken from elective pathway transformation work undertaken around the world. Implementation could happen in parallel with the work being done on the emergency response and will be critical to the Kingdom, minimizing the direct and indirect mortality from Covid-19, together with the time taken for the system to return to normal.
Graham Jelley

Director - Healthcare
KPMG in Saudi Arabia
Connect with us
- Find office locations kpmg.findOfficeLocations
- kpmg.emailUs
- Social media @ KPMG kpmg.socialMedia

